Selenium exposure in the diet and in supplements: in this review article, we summarize the key outcomes of the best selenium exposure studies.
Optimal Selenium Intake and Status
In his review of the available research literature, Professor Urban Alehagen, Linköping University, Sweden, concluded that a daily intake of 100–150 mcg of selenium per day is required.
This is the intake level that enables an optimal expression of the important selenoprotein P that transports selenium from the liver to peripheral tissues [Alehagen 2022]. For other selenoproteins to be optimized, i.e., to be fully expressed, Prof. Alehagen argues that selenium status of approximately 120 mcg/L when measured in red blood cells is necessary [Alehagen 2022].
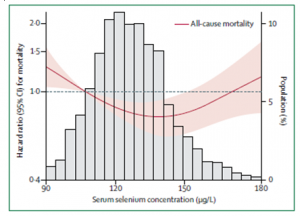
Professor Margaret P. Rayman, University of Surrey, United Kingdom, has advanced the idea of a U-shaped relationship between selenium intake/status and health. According to her analysis, the lowest risk of all-cause mortality seems to lie in the range 120-150 mcg/L of serum selenium [Rayman 2012; Rayman 2020].
Deficient Selenium Intake and Status
In the BIOSTAT-CHF Study, a multinational, prospective, observational cohort study that enrolled patients with worsening heart failure, Dr. Nils Bomer and a research team led by Prof. Peter van der Meer showed that heart failure patients with a serum selenium concentration of less than 70 mcg/L (deficiency status) had significantly worse clinical signs and symptoms [Bomer 2020]:
- worse New York Heart Association functional class
- more severe signs and symptoms of heart failure
- poorer exercise capacity (6-min walking test)
- poorer quality of life (Kansas City Cardiomyopathy Questionnaire)
The selenium deficiency was associated with significantly higher rates of the primary endpoint: a composite of all-cause mortality and hospitalization for heart failure. Selenium deficiency in heart failure patients is independently associated with impaired exercise tolerance and with a 50% higher mortality rate [Bomer 2020].
Heart failure patients with serum concentrations of 70–100 mcg/L appeared to have similar adverse associations, suggesting that values below 100 mcg/L might be considered abnormal [Bomer 2020].
Optimal Form of Selenium Supplement
In a randomized, double-blind, placebo-controlled trial of selenium yeast (200 or 285 mcg/day) or pure selenomethionine (200 mcg/day) administered for 9 months in 69 healthy men, the plasma selenium concentrations increased as follows [Richie 2014]:
- 93% in the selenomethionine group
- 54% in the low selenium yeast group
- 86% in the high selenium yeast group
The Pennsylvania State University researchers used a high-dose selenium yeast – 285 mcg – because it contained 200 mcg selenium corresponding to 200 mcg selenium in the pure selenomethionine product.
After a 3-month washout, the plasma selenium levels returned to baseline levels.
The noteworthy outcome in the study was that the two selenium yeast treatments were significantly associated with reductions in biomarkers of oxidative stress; the pure selenomethionine supplementation was not [Richie 2014].
The study findings suggest that selenium-containing compounds in the selenium yeast other than selenomethionine may account for the decrease in oxidative stress [Richie 2014].
Establishing Optimal Selenium Intakes and Status
In a seminal study, Rachel Hurst and a research group led by Prof. Susan J Fairweather-Tait, University of East Anglia, United Kingdom, found that that 50, 100, or 200 micrograms of selenium from selenium yeast supplements daily in addition to approximately 55 micrograms of selenium daily from food for 10 weeks will raise the plasma selenium levels as follows [Hurst 2010]:
- From 95.7 micrograms per liter up to 118.3 micrograms per liter with a daily selenium supplement of 50 micrograms
- From 95.7 micrograms per liter up to 152.0 micrograms per liter with a daily selenium supplement of 100 micrograms
- From 95.7 micrograms per liter up to 177.4 micrograms per liter with a daily selenium supplement of 200 micrograms
In the KiSel-10 Study of four years of daily combined supplementation of healthy elderly citizens with 200 mcg of selenium in selenium yeast and 200 milligrams of Coenzyme Q10, Prof. Alehagen showed the following effect of the supplementation with selenium yeast [Alehagen 2020]:
- The baseline serum selenium level was 67.1 mcg/L, corresponding to an estimated daily selenium intake of 35 mcg.
- The post-intervention selenium concentrations were 210 mcg/L in the active treatment group and 72 mcg/L in the placebo group.
Meta-Analyses of Selenium Exposure and Cancer Risk

In a meta-analysis of 37 population-based prospective studies, Kuria et al found that there was an inverse relationship between selenium intake and overall cancer risk after adjusting for age, body mass index, and smoking.
The meta-analysis findings suggest that selenium is protective against cancer; however, the effects vary with different cancers [Kuria 2020].
In a meta-analysis of 38 studies enrolling 36,419 prostate cancer cases and 105,293 controls, Sayehmiri et al found that the pooled relative risk of the relationship between selenium and prostate cancer was 0.86 = a 14% reduction in the risk of prostate cancer associated with higher selenium status [Sayehmiri 2018].
- Case-control studies: 11% risk reduction
- Cohort studies: 23% risk reduction
- Randomized controlled studies: 10% risk reduction
In 10 studies of selenium status and advanced prostate cancer, the relative risk of advanced prostate cancer was 33% lower with higher selenium status [Sayehmiri 2018].
In a meta-analysis of 69 observational studies, Cai et al found that the extent of selenium exposure has different effects on different types of cancer. Higher selenium exposure was associated with decreased risk of breast cancer, lung cancer, esophageal cancer, gastric cancer, and prostate cancer but was not associated with reductions in the incidence of colorectal cancer, bladder cancer, and skin cancer [Cai 2016].
In a systematic review and meta-analysis of 12 studies with a total of 13,254 participants and 5007 cases of prostate cancer, Hurst et al showed that the prostate cancer risk decreased with increasing plasma/serum selenium status from 60 mcg/L up to 170 mcg/L [Hurst 2012].
Meta-Analyses of Selenium Exposure and Heart Disease Risk
In a meta-analysis of 13 observational studies and randomized controlled trials, Kuria et al found that, overall, selenium status is associated with a reduced risk of cardiovascular disease incidence (RR = 0.66) and cardiovascular disease mortality (RR = 0.69) in physiologically high selenium status compared to low selenium status in the body [Kuria 2021].
The data showed that there was a 15% reduced risk of cardiovascular disease incidence per 10 mcg increment in blood selenium concentration.
Physiologically high selenium levels in the body were associated with decreased risk for cardiovascular disease incidence and mortality [Kuria 2021].
Data from the KiSel-10 Study indicate the possible biological mechanisms by which combined selenium and Coenzyme Q10 supplementation can reduce the risk of death from cardiovascular disease [Alehagen 2018]:
- reduced plasma bio-markers of inflammation
- reduced plasma bio-markers of oxidative stress
- reduced plasma bio-markers of fibrosis.
In the study, a randomized controlled trial, researchers in Sweden gave healthy elderly individuals 200 mcg selenium as selenium yeast tablets together with 200 mg ubiquinone CoQ10 supplements daily for four years. The combined selenium and CoQ10 treatment was associated with reduced cardiovascular mortality and improved heart function, The reduced cardiovascular mortality persisted in the active treatment group for eight years of follow-up after the cessation of supplementation [Alehagen 2018].
Selenium Exposure and COVID-19 Cure Rate
A comparison of selenium status (using selenium status data from hair measurements) with recovery rates from COVID-19 in 17 Chinese cities has shown that COVID-19 cure-rates were higher and COVID-19 death-rates were lower in areas in which the population had higher selenium concentrations [Zhang 2020].
Selenium Exposure and Type-2 Diabetes Risk
In a review article, Prof. Lutz Schomburg, Charité, Berlin, Germany, explains that the “… current data show that supplemental Se does not cause diabetes.”
Prof. Schomburg explains that the best explanation for an association between high plasma/serum selenium concentrations and elevated incidence of type-2 diabetes is that diabetes potentially causes increased hepatic selenoprotein P biosynthesis and causally raises circulating selenium and selenoprotein P levels. He explains that, under normal conditions, insulin decreases selenoprotein P biosynthesis and secretion. In cases of insulin resistance, this inhibition declines, causing higher circulating selenium concentrations and higher selenoprotein P levels [Schomburg 2020].
According to Prof. Schomburg, it is likely that high selenium status does not increase diabetes risk but that diabetes causes increasing selenoprotein P levels. “In the later stages of diabetes type 2, when insulin levels decrease due to a progressive decline in β-cell function, the high glucose concentrations still promote selenoprotein P biosynthesis and secretion if these are not counteracted by medication, e.g., with metformin” [Schomburg 2020].
Kohler et al conducted a review of 16 studies, 13 observational studies and 3 RCTs. 8 of the 13 observational studies showed a statistically significant positive association between concentrations of selenium and odds for type-2 diabetes. In contrast, among RCTs of selenium, a higher risk of type-2 diabetes was not observed for those who received selenium compared to a placebo [Kohler 2018].
Selenium Exposure and Mercury Toxicity
Research indicates that methylmercury (CH3Hg+) irreversibly inhibits the synthesis and activity of the selenoenzymes that normally prevent/reverse oxidative damage in the brain. Unless supplemental selenium is provided, the consequences increase as the quantity of the CH3Hg+ approaches and exceeds the available quantities of selenium, inducing a conditioned selenium deficiency [Ralston 2018]. It is the disruption of selenium biochemistry that characterizes mercury neurotoxicity.
Selenium Exposure and Thyroid Health
The situation with respect to selenium exposure and thyroid health is complicated. On the one hand, persistent low selenium intake is associated with increased thyroid disease risk [Schomburg 2020]. On the other hand, the thyroid gland has high priority for the supply of selenium, which makes it unlikely that selenium status and selenoprotein expression in thyroid gland cells is affected by small differences in dietary selenium intakes [Schomburg 2020]. Even so, some studies show that patients with Hashimoto’s thyroiditis, Graves’ disease, or Graves’ orbitopathy do respond positively to selenium supplementation [Schomburg 2020].
In contrast to the thyroid gland, the immune system does not get a high-priority supply of selenium in times of selenium deficiency. Consequently, the immune response to a challenge may be inadequate because of insufficiently expressed and active selenoproteins. There may be a suboptimal interaction between thyroid gland cells and immune system lymphocytes whenever there is a challenge by infection, trauma, shock, or other toxic effects [Schomburg 2020].
Conclusion: Adequate Selenium Exposure is Essential for Good Health
Selenium from the diet and from supplements: there seems to be a U-shaped relationship between selenium exposure and health such that a serum selenium concentration of ca. 125 mcg/L is optimal for good health and lower risk of all-cause mortality.
Sources
Alehagen U, Johansson P, Svensson E, Aaseth J, Alexander J. Improved cardiovascular health by supplementation with selenium and coenzyme Q10: applying structural equation modelling (SEM) to clinical outcomes and biomarkers to explore underlying mechanisms in a prospective randomized double-blind placebo-controlled intervention project in Sweden. Eur J Nutr. 2022 Apr 6. doi: 10.1007/s00394-022-02876-1. Epub ahead of print.
Alehagen U, Aaseth J, Alexander J, Johansson P, Larsson A. Supplemental selenium and coenzyme Q10 reduce glycation along with cardiovascular mortality in an elderly population with low selenium status – A four-year, prospective, randomised, double-blind placebo-controlled trial. J Trace Elem Med Biol. 2020 May 4;61:126541.
Alehagen U, Johansson P, Björnstedt M, Rosén A, Dahlström U. Cardiovascular mortality and N-terminal-proBNP reduced after combined selenium and coenzyme Q10 supplementation: a 5-year prospective randomized double-blind placebo-controlled trial among elderly Swedish citizens. Int J Cardiol. 2013 Sep 1;167(5):1860-6.
Alehagen U, Aaseth J, Alexander J, Johansson P. Still reduced cardiovascular mortality 12 years after supplementation with selenium and coenzyme Q10 for four years: A validation of previous 10-year follow-up results of a prospective randomized controlled trial. PLoS One. 2018;13:e0193120.
Bomer N, Grote Beverborg N, Hoes MF, Streng KW, Vermeer M, Dokter MM, IJmker J, Anker SD, Cleland JGF, Hillege HL, Lang CC, Ng LL, Samani NJ, Tromp J, van Veldhuisen DJ, Touw DJ, Voors AA, van der Meer P. Selenium and outcome in heart failure. Eur J Heart Fail. 2020 Aug;22(8):1415-1423.
Cai X, Wang C, Yu W, Fan W, Wang S, Shen N, Wu P, Li X, Wang F. Selenium exposure and cancer risk: An updated meta-analysis and meta-regression. Sci Rep. 2016 Jan 20;6:19213.
Hurst, R., Armah, C.N., Dainty J.R., Hart, D.J., Teucher, B., Goldson, A.J., Broadley, M.R., Motley, A.K., Fairweather-Tait, S.J. Establishing optimal selenium status: results of a randomized, double-blind, placebo-controlled trial. Am J Clin Nutr. 2010;91(4):923-31.
Hurst R, Hooper L, Norat T, Lau R, Aune D, Greenwood DC, Vieira R, Collings R, Harvey LJ, Sterne JA, Beynon R, Savović J, Fairweather-Tait SJ. Selenium and prostate cancer: systematic review and meta-analysis. Am J Clin Nutr. 2012 Jul;96(1):111-22.
Kohler LN, Foote J, Kelley CP, et al. Selenium and Type 2 Diabetes: Systematic Review. Nutrients. 2018;10(12):1924. Published 2018 Dec 5.
Kuria A, Fang X, Li M, Han H, He J, Aaseth JO, Cao Y. Does dietary intake of selenium protect against cancer? A systematic review and meta-analysis of population-based prospective studies. Crit Rev Food Sci Nutr. 2020;60(4):684-694.
Kuria A, Tian H, Li M, Wang Y, Aaseth JO, Zang J, Cao Y. Selenium status in the body and cardiovascular disease: a systematic review and meta-analysis. Crit Rev Food Sci Nutr. 2021;61(21):3616-3625.
Ralston NVC, Raymond LJ. Mercury’s neurotoxicity is characterized by its disruption of selenium biochemistry. Biochim Biophys Acta Gen Subj. 2018 Nov;1862(11):2405-2416.
Rayman MP. Selenium intake, status, and health: a complex relationship. Hormones (Athens). 2020;19(1):9-14.
Rayman MP. Selenium and human health. Lancet. 2012 Mar 31;379(9822):1256-68.
Richie JP Jr, Das A, Calcagnotto AM, et al. Comparative effects of two different forms of selenium on oxidative stress biomarkers in healthy men: a randomized clinical trial. Cancer Prev Res (Phila). 2014;7(8):796-804.
Sayehmiri K, Azami M, Mohammadi Y, Soleymani A, Tardeh Z. The association between selenium and prostate cancer: a systematic review and meta-analysis. Asian Pac J Cancer Prev. 2018 Jun 25;19(6):1431-1437.
Schomburg L. The other view: the trace element selenium as a micronutrient in thyroid disease, diabetes, and beyond. Hormones (Athens). 2020 Mar;19(1):15-24.
Zhang J, Taylor EW, Bennett K, Saad R, Rayman MP. Association between regional selenium status and reported outcome of COVID-19 cases in China. Am J Clin Nutr. 2020;11:1297–9.
The information presented in this review article is not intended as medical advice and should not be used as such.
28 July 2022
